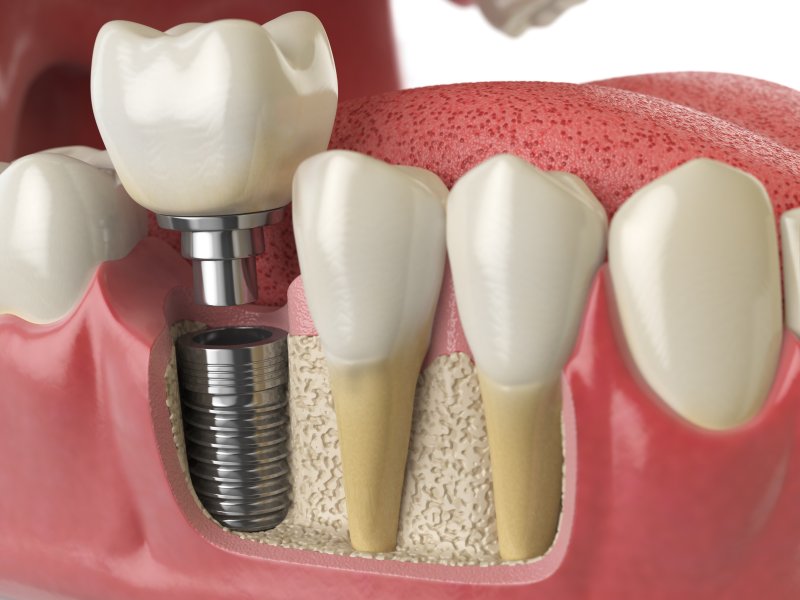
Bruxism, a habitual grinding or clenching of the teeth, can pose significant challenges for dental implant restorations. The repeated forces generated by bruxism can lead to implant overload, bone loss, and restoration failure, compromising the long-term success of dental implant restorations. As a provider of dental implant restorations in Pekin, it’s essential to recognize the unique needs and considerations of patients with bruxism.
In this article, we’ll explore the clinical considerations and treatment strategies for dental implant restorations in patients with bruxism.
What is Bruxism?
Bruxism is a habitual grinding or clenching of the teeth that can occur during the day or at night. It is a complex condition that involves the coordination of the jaw muscles, teeth, and nervous system. Bruxism can manifest in different ways, including grinding or clenching of the teeth, clicking or snapping of the jaw, and even facial pain or headaches. It can be triggered by various factors, such as stress, anxiety, or misalignment of the teeth or jaw.
Bruxism can lead to a range of problems, including tooth wear, jaw pain, and damage to dental restorations or implants.
Clinical Considerations
Patients with bruxism present several clinical challenges when it comes to dental implant restorations. These include:
- Increased occlusal forces: Bruxism generates excessive occlusal forces that can lead to implant overload, screw loosening, and prosthetic fracture.
- Bone loss and density changes: Chronic bruxism can lead to bone loss and density changes, which can compromise implant stability and osseointegration.
- Prosthetic complications: Bruxism can cause prosthetic complications, such as chipping, cracking, or fracture of the implant-supported restoration.
- Patient compliance: Patients with bruxism may have difficulty complying with post-operative instructions, such as avoiding hard or sticky foods, which can compromise implant success.
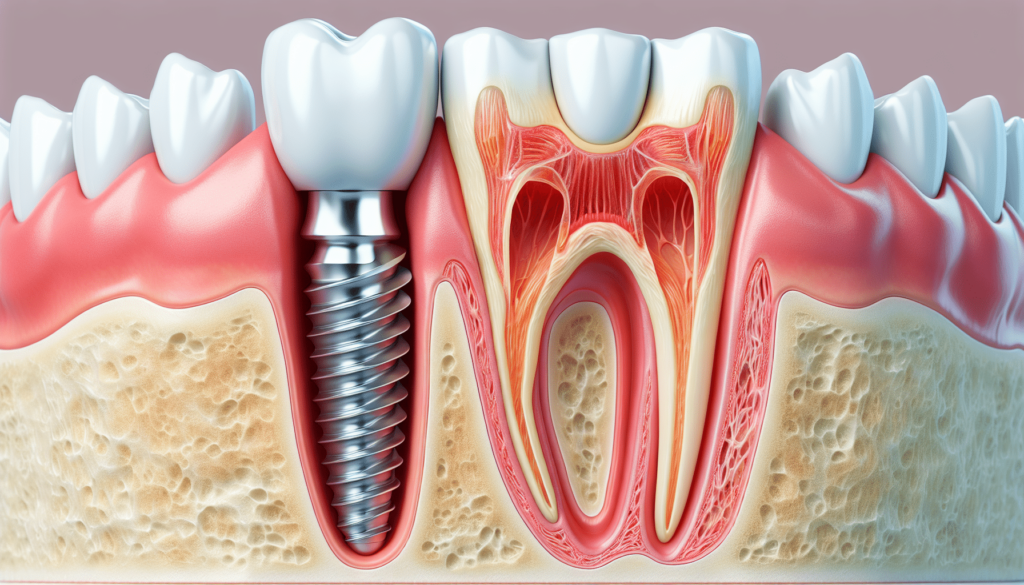
Diagnosis And Treatment Planning
Accurate diagnosis and treatment planning are critical when it comes to dental implant restorations in patients with bruxism. The following steps should be taken:
- Clinical examination: A thorough clinical examination should be performed to assess the patient’s occlusion, jaw alignment, and overall oral health.
- Radiographic evaluation: Radiographs should be taken to evaluate bone density, implant placement, and prosthetic design.
- Bruxism assessment: A bruxism assessment should be performed to determine the severity of the condition and identify potential triggers.
- Treatment planning: A comprehensive treatment plan should be developed, taking into account the patient’s bruxism, occlusal scheme, and prosthetic needs.
Exploring Effective Treatment Options
Several treatment options are available for dental implant restorations in patients with bruxism. These include:
- Implant design and placement: Implants should be designed and placed to withstand the excessive occlusal forces generated by bruxism.
- Prosthetic design and materials: Prosthetic design and materials should be selected to minimize the risk of chipping, cracking, or fracture.
- Occlusal adjustment and equilibration: Occlusal adjustment and equilibration should be performed to distribute occlusal forces evenly and reduce the risk of implant overload.
- Night guards and splints: Night guards and splints can be used to protect the implant-supported restoration from excessive occlusal forces during sleep.
Case Management and Follow-Up
Effective case management and follow-up are critical to ensuring the long-term success of dental implant restorations in patients with bruxism. The following steps should be taken:
- Regular follow-up appointments: Regular follow-up appointments should be scheduled to monitor implant stability, prosthetic function, and patient compliance.
- Occlusal adjustment and equilibration: Occlusal adjustment and equilibration should be performed as needed to maintain optimal occlusal function and reduce the risk of implant overload.
- Prosthetic maintenance and repair: Prosthetic maintenance and repair should be performed as needed to ensure the continued function and aesthetics of the implant-supported restoration.
By understanding the clinical considerations and challenges associated with bruxism, clinicians can develop effective treatment plans that minimize the risk of implant failure, screw loosening, and prosthetic fracture. Regular follow-up appointments and occlusal adjustment and equilibration are critical to ensuring the long-term success of dental implant restorations in patients with bruxism.